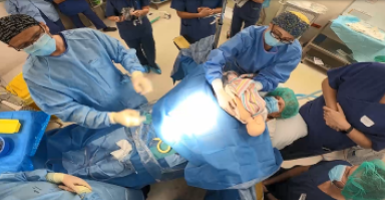
Capturing ‘Work as Done’ with Mater Education’s OptiSim program
 Blog written by Brooke Dench; Registered Nurse, Human Factors Advisor at Mater Education
Blog written by Brooke Dench; Registered Nurse, Human Factors Advisor at Mater Education
Throughout my patient safety and quality roles, I have assisted many clinical teams to design or redesign clinical processes. Whilst this may sound easy, there are many challenges in embedding a safe and efficient process into a busy, unpredictable clinical environment.
Often process redesign is a tabletop exercise, with clinicians coming together to discuss how a process can look. We rely on the clinical experts around the table to predict how the particular process will behave across a 24/7 time period and across multidisciplinary teams, with varying experience. We expect the clinicians to guide us on understanding how the interconnecting systems and processes will be impacted and behave in response to the introduction of this new way of working.
I don’t know what your thoughts are, but I think WOW, we are asking a lot from these clinicians! Don’t get me wrong, these are highly intelligent capable clinicians, but in a system as complex as healthcare, there is no way to accurately predict system behaviour when discussed around a table. I don’t ever recall a nursing shift that was ever the same day to day. There were always different challenges, some that you could never predict. This tabletop planning uses a concept termed ‘Work as Imagined’. We make assumptions on how the people, the system and the environment will interact. These assumptions are also fraught with our own cognitive biases based on past experience; we are of course human after all.
I was first introduced to the concept of Work as Imagined whilst studying for my Masters in Human Factors and Organisational Behaviour. It really opened my eyes, and I have never been able to view a health system the same again! Human factors allow us to understand how humans interact with their environment, with other people and with the systems around them (International Ergonomics Association, 2019). By understanding the systems in which humans work we can design better systems, processes and environments to minimise the chance for error. The main aim of Human factors is to enhance the safety and wellbeing of all users and optimise the performance of the system. As the healthcare industry has a high error and harm rate (WHO, 2013) and poorly designed systems, the implementation of human factors (by qualified Human Factors practitioners) into healthcare has never been so critical.
Another important consideration when designing a system is ‘Work as Prescribed’. We are bound by many policies and procedures in healthcare; but do they align with how things actually work? It is likely they don’t! Policies and procedures prescribe the way we should be working but often they are built on the foundations of work as imagined. They prescribe work in a linear fashion; however we know that complex systems don’t work in a linear fashion. There are many things occurring simultaneously and due to the highly variable nature of healthcare, policies don’t capture and prescribe all the variations that are likely to occur and the required actions, again failing to capture how work is actually done in the real world clinical setting.
So how do we overcome work as imagined and prescribed to ensure that our systems, processes and clinicians are functioning at their absolute best in a minimalist risk approach to our patients? Well, that’s where we need to understand ‘Work as Done’. This is where we go out to the clinical areas and we observe and measure exactly how things work, or could work. Understanding work as done allows us to test the assumptions we made when planning the new process to ensure that the process is going to work. We can determine if there are workarounds required in order for clinicians to achieve their goals. We can directly observe the interactions between people, the environment and the process and identify potential sources of error and risk and thereby making the healthcare system safer for our patients.
I have recently been involved in understanding work as done as part of Mater Education’s OptiSim program. OptiSim, Optimisation through Simulation, uses medical simulation to recreate the real world experience within the clinical environment. With OptiSim we can take new processes and procedures and test them in the clinical environment with clinicians prior to implementation, to ensure that everything runs smoothly and the process is as safe and low risk as possible. It has been specifically designed to test new or repurposed environments, equipment and processes. OptiSim turns the work as imagined and prescribed into work as done.
To date, Mater Education has performed more than 30 OptiSim activities, resulting in close to 100 individual simulations, ranging from testing a greenfield hospital site, to procedural rehearsals and new process tests. In each instance of these simulations there has been a range of issues that were not considered during the planning stage, some of which could have had serious consequences if they had not been picked up prior to implementation.
I was lucky enough to be involved in the testing of Mater Mothers’ Private Brisbane’s new offering, Mater Moments at the Emporium. Mater Moments at Emporium is available to mums who would like to spend precious time with the latest addition to their family in elegant, stylish surrounds at Emporium Hotel South Bank before heading home.
We tested this new process prior to opening the service to ensure that our mothers were going to have the best possible experience. We had the team of Mater Mothers’ Private Brisbane clinicians and administration staff test the process; from the discharge planning phase and discharge process from hospital, to the transfer of mother and baby to the Emporium Hotel South Bank in a luxury transfer. Our OptiSim team then tested the process and a range of emergency scenarios with Emporium staff and the Mater midwife that would be based at the Emporium.
Just as all other OptiSim tests had picked up potential issues, this process too had issues that had to be re-considered prior to implementation. Whilst only minor in this scenario, they have the potential to impact on the experience of both our patients and family, and our staff satisfaction. This new process was in no doubt designed really well; the attention to detail around the experience of the mother was exceptional. Where we ran into some potential issues, and this is not uncommon, was where other systems need to interact with our newly designed process. How does our normal discharge process interact? How does flawless communication happen between wards and key personnel? Do the midwives have all the information they need to inform the patient of the process? Often when we introduce a new process amongst our other processes, it can disrupt the flow of how the work is normally done. In this case, we needed to slightly tweak how discharge is considered, to design a communication flow and board to share information between key stakeholders, and update our marketing brochure with information that had been previously overlooked. The only way we could have known that we needed to make changes prior to implementation was by utilising Mater Education’s OptiSim service and testing this process in the real world setting to see how work is done!
The team at Mater Mothers’ Private Brisbane can now be assured that this process will be close to optimal performance from day one of implementation, and that our patients will have an exceptional experience. The new service has been tried and tested prior to patient utilisation and the potential ‘teething’ problems normally experienced with the opening of a new service have been minimised. We have bridged the gap between work as imagined, work as prescribed and work as done through the use of OptiSim; Mater Education’s simulated process testing program.
To find out more about Mater Education’s OptiSim contact the team here.
You can also read about Mater Education’s documentation framework for simulation quality improvement activities.
About the Author
Brooke Dench is a Human Factors Advisor for Mater Education and a Quality By Design Partner for Mater Health Services. Using her extensive experience in healthcare quality and safety, Brooke has facilitated and led clinical investigations, improvements, system and process redesign and testing with a range of healthcare professionals. Brooke is a Registered Nurse with post graduate qualifications in critical care, holds an Honours in Psychology and a Masters in Human Factors/Ergonomics and Organisational Behaviour. Brooke has a vision to transform patient safety programs by embedding the use of human factors into healthcare safety and quality programs.
References
International Ergonomics Association, 2019. Definition and Domains of Ergonomics. Retrieved from website: https://www.iea.cc/whats/index.html
WHO. (2013). World Health Organization. Patient safety. 2013. Retrieved from website: http://www.who.int/patientsafety/about/en.